Kuka came to the hospital unconscious and barely breathing. She had been struck by a motor vehicle while walking along the side of the road. During my initial exam, I did not find much in terms of trauma except for some blood on her scalp. I watched as her motionless, five-year-old tiny body intermittently tensed and contorted into postures consistent with severe brain damage. Even in a more modern hospital with a pediatric neurosurgeon, Kuka’s injury pattern would likely have a poor prognosis.
We did what we could for her. We put a tube down her trachea, breathed for her, and gave her oxygen. We got X-rays and did an ultrasound, but without a CT scan, we could not diagnose the most likely source of her current state – a devastating head injury. Unfortunately, I was almost positive that Kuka would die, especially with our limited resources. I spoke with our surgeons to see if they could do anything, and after some discussion, they decided to take her to the operating theater (OT). We had low expectations for a positive outcome, but we would try what we could.
In the OT our two surgeons, Dr. Ben and Dr. Sheryl, drilled two burr holes on each side of Kuka’s head with a sterilized power drill. After drilling through the skull on both sides, they discovered bilateral epidural hematomas, blood layering on both sides of the head just under the skull. Almost immediately after surgery, Kuka showed signs of improvement. The next morning Kuka was nearly back to normal, and seven days after this horrifying incident, she was discharged a normal, happy little girl!
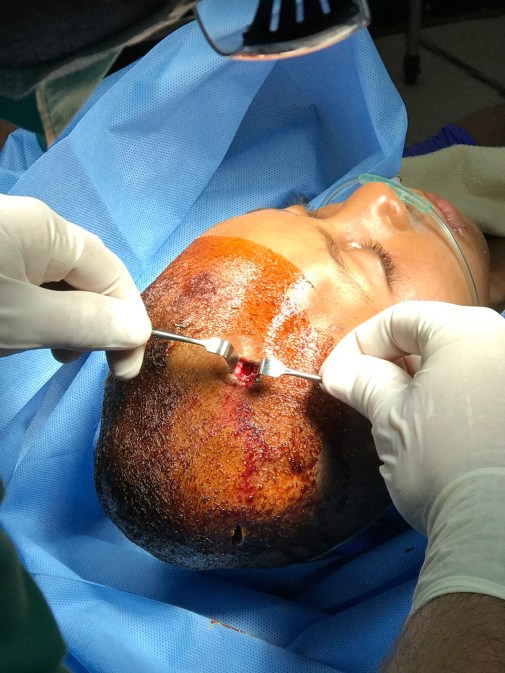
Practicing at a hospital in an underdeveloped nation forces you to work outside of your comfort zone. During my time in Papua New Guinea, I have learned to diagnose and manage medical problems that would be done solely by a specialist or sub-specialist in the United States. High risk obstetrics, neonatal ICU, strange infectious diseases, seizure disorders, oncology, and autoimmune diseases are just a few examples of the many things I have had to learn how to treat. Likewise, in the trauma center where I trained, even a neurosurgeon with state-of-the-art equipment and a CT scan to guide his drill would have been uncomfortable managing Kuka. Most American hospitals would have flown Kuka by helicopter to the nearest Pediatric Hospital to be treated by a Pediatric Neurosurgeon.
I feel very blessed to work with such an amazing team who will do things outside of their training and comfort zone to help patients who are in their greatest need. People like Ben, Sheryl, and the other medical doctors here have taught me a great deal about medicine. But even more importantly, they’ve modeled how to trust God in situations that are beyond our control. There is no residency program that could completely prepare me for everything that emerges on the mission field. However, during these critical moments, we face our inadequacies and learn to trust God to guide us and shine through our weaknesses.

As Hudson Taylor, a 19th century missionary to China, said,
“God uses men who are weak and feeble enough to lean on Him.”
“But he said to me, ‘My grace is sufficient for you, for my power is made perfect in weakness.’ Therefore I will boast all the more gladly about my weaknesses, so that Christ’s power may rest on me.”
– 1 Corinthians 12:9
God bless you and the other doctors for what you are doing. Sending a lot of prayers too.
LikeLike
What a great ‘feel good’ story to start the day!
LikeLike
What a great story! I love what God is doing to other peoples lives through you! I pass by your former residence almost everyday in Erie and I do pray for you. Also, Im still keeping the ball your son gave to me and I have it in my car as I type this! God bless you so much for all what you are doing!
Morris the Kenyan in Erie!
LikeLike
Reblogged this on morrismunenemugo.
LikeLike